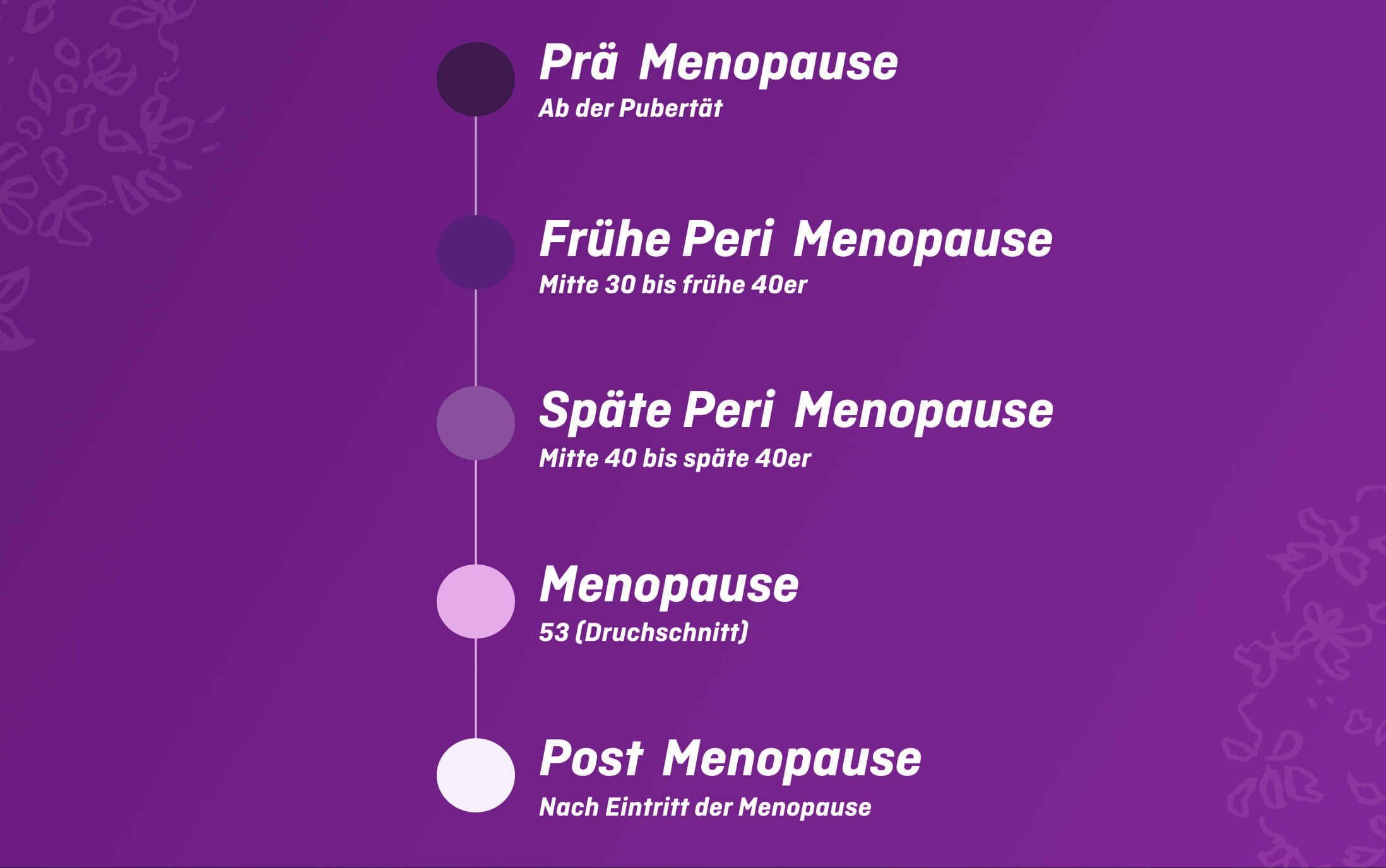
Thrush during the menopause
Thrush is nothing unusual, with three-quarters of all women having experienced these kinds of complaints at least once. Thrush is easy to recognise: the vagina burns and itches, there is a white coating on the vagina and the discharge is white, sometimes crumbly. Read more in this article to find out what thrush is, how it manifests, what facilitates it and what you can do about it.
Thrush during the menopause: Signs and symptoms
Vaginal infections and vaginitis are some of the most common gynaecological illnesses and can occur in women of all ages. Almost every woman experiences them at some point. They often occur in sexually active and pregnant women, but the oestrogen deficiency during the menopause also facilitates these complaints. Thrush usually results in vaginitis (also known as colpitis), with so-called “bacterial vaginosis” generally occurring without vaginitis.

A side note: In the medical world, the suffix -ose is used for a non-inflammatory and -itis for an inflammatory illness.
Almost every woman gets vaginitis at some point, with it often occurring in women with hormonal fluctuations, such as pregnant women. The pill and oestrogen deficiency during the menopause also facilitate vaginitis. Stress and excessively intense vaginal hygiene can also be responsible for thrush. Vaginitis is generally triggered by yeast fungi, which is usually already present in the vagina and can gain the upper hand through various influences or can also be caused externally through unprotected sex or incorrect vaginal hygiene.
Menopausal and postmenopausal women are more susceptible to vaginitis and vaginal infections. This is due to various reasons. Hormonal changes in the menopause can cause the pH value in the vaginal environment to increase and the natural acid resistance to weaken, enabling pathogenic germs in the vagina to prevail more easily and increase susceptibility for vaginitis.
A further consequence of the falling oestrogen level during the menopause is that the vaginal mucosa (known as atrophy) becomes thinner. This goes hand in hand with increased susceptibility to vaginal inflammations and infections. Atrophic vaginitis (also known as atrophic colpitis) occurs particularly during the postmenopause or in women who have already had their oestrogen production inhibited through medication or operations, such as during cancer treatment.
Atrophic vaginitis occurs particularly during the postmenopause.
Thrush during the menopause – What you need to know
Thrush mainly occurs in women of reproductive age. Thrush is the most common kind of vaginal infection and is known medically as vaginal mycosis (i.e. fungal infection). One technical term is commonly vaginal candidiasis, as the main pathogen is the yeast fungus Candida albicans.
Typical signs are white, sometimes crumbly discharge, swelling and reddening of the vaginal mucosa with white coatings, accompanied by itching and burning.
Risk factors include unprotected sexual intercourse, oral contraceptives (i.e. the pill), Diabetes mellitus, an overactive or underactive thyroid or immunosuppressive therapy. Particularly after therapy with antibiotics, the risk of thrush is significantly elevated.
Around 75% of all women have had vaginal mycosis at least once in their lives.
Around 5% develop a form that recurs several times a year (recurring infection).
Thrush during the menopause – Prevention and treatment
There are several things you can do to prevent vaginitis. But first, it is important to understand the vaginal balance.
A healthy vagina has a natural balance, which is maintained by the natural acid resistance and natural vaginal moisture and can sometimes be disrupted by different influences.
In the healthy vagina, a high amount of lactic acid bacteria are at work. They work hard to produce lactic acid and hydrogen peroxide (H2O2). Undesirable pathogens do not stand a chance in this acidic, antibiotic environment. The vaginal balance protects the vagina against infections. In order to fulfil this important task, the lactic acid bacteria rely on natural moisture. For this reason, women with vaginal dryness are more susceptible to vaginal infections.

Thrush – Prevention
The vaginal balance can be supported by a suitable diet (such as prebiotics, probiotics and refraining from excessive carbohydrate consumption) and sufficient liquid intake with healthy drinks such as water or tea and, if any risk factors are present or there is a tendency towards vaginitis, strengthened or restored using acidifying remedies.
There are some tips you should know if you have a tendency towards thrush:
Avoid unprotected sex: Disruptions to the vaginal environment are mainly widespread in sexually active women. Sperm weakens the vaginal acid resistance due to its higher pH value. For this reason, you should avoid unprotected sex, especially if you are at higher risk of vaginitis.
Wear suitable clothing: Fungi like a moist, warm environment. Therefore wear air-permeable, cotton underwear, which you can wash at 60 degrees. Whenever you go swimming, you should change your wet swimsuit or bikini quickly.
Try probiotics: With a predisposition to thrush, probiotics containing lactobacilli (that is, a specific type of lactic acid bacteria) can help to restore the natural vaginal flora and are mainly recommended with recurring infections.
Avoid carbohydrates: Fungi love carbohydrates. If you tend towards infections with yeast fungi, you should check your carbohydrate consumption, as a carbohydrate-focused diet can facilitate fungal infections. Avoid or reduce sugar if possible, as well as all simple carbohydrates such as pasta, rice and white bread. The fruit sugar and alcohol contained in fruit are also beneficial for yeast fungi and should therefore be consumed sparingly.
Bacterial vaginosis or thrush? How to tell the difference.
|
|
|
|
|---|---|---|
|
Vaginal discharge |
Increase in grey-white to yellow, thin discharge |
Whitish, thick, partially crumbly discharge |
|
Vagina smell |
Typically fishy, sometimes even sweet |
Unspecific |
|
Complaints |
Sometimes burning when urinating or having sex |
Typically vaginitis with swelling and reddening of the vaginal mucosa with white coatings, accompanied by itching and burning. |
menoelle® and vaginal mycosis
If you frequently suffer from thrush or have a predisposition to do so, it may be sensible to make a preventive treatment with an acidifying product specially tailored to the vaginal flora to support the natural acid resistance and restoration of the vaginal balance. For menopausal women with accompanying vaginal dryness as a possible cause, it is advised to combine these with moisturising remedies.
menoelle® OVULA med is a medical product that helps maintain the natural defences of the vagina and promotes the restoration of healthy vaginal flora.
Lactic acid, normally present in the vagina, favours an immediate pH correction and facilitates the natural recovery of the delicate vulvo-vaginal ecosystem. Boric acid, thanks to its persistence in the vaginal environment, favours a lowering of pH prolonged over time.
Hyaluronic acid exerts a hydrating and lubricating action against vaginal dryness and helps to restore a natural and comfortable vaginal environment.
A treatment with menoelle® OVULA med vaginal suppositories can restore and preserve vaginal health.
Cue: Visit the doctor
You can treat thrush easily, which is easy to distinguish from a bacterial vaginosis or other vaginal infections, with over-the-counter medication if needed. Nevertheless, it is worth visiting your gynaecologist, as vaginal itching is only caused by an acute vaginal fungal infection in around one-third of cases, particularly if no other typical indications for thrush exist.
Often, a vulvodynia is present instead, which, among other things, can be caused by preceding infections with thrush. Therefore make sure to treat thrush quickly to prevent the vaginal mycosis developing into something chronic and recurring.
Over-the-counter acidifying remedies are usually not suitable for fighting acute vaginitis.

Menotest
menoelle®-menopause test
Am I already in the menopause or not yet?
Simply answer the 20 short questions in our menoelle® menopause test to know more straight away.